Leading with Love: Starting the Conversation on Residential Treatment
Leading with Love: Starting the Conversation on Residential Treatment
By Juliana Pang

Juliana Pang
Juliana is a Registered Counsellor and Clinical Member of the Singapore Association for Counselling, with a master’s degree in counselling from Monash University. As one of The Winslow’s psychotherapists, she supports clients and their loved ones through the challenges of recovery.
There comes a time when family members realise that their loved one who has been struggling with addiction is unable to stop on their own, not even with some level of outpatient professional help. There may have been countless conversations about seeking residential treatment, but your loved one continues to refuse this option. You are feeling a sense of exasperation and powerlessness as you watch your loved one spiral towards destruction, with no clear guidance on what you could do next.
Over the course of my work with families navigating this deeply difficult situation, I have observed that there is no perfect script, no magic combination of words that guarantees the outcome one hopes for. But there are principles grounded in clinical experience and a clear understanding of how addiction works that can guide these conversations.
Understand the Disease That Has Entrapped Your Loved One
American Society of Addiction Medicine (ASAM) classifies addiction as a “treatable, chronic medical disease involving complex interactions among brain circuits, genetics, the environment, and an individual’s life experiences.”
In simple terms, addiction is not a result of a lack of willpower, nor a moral failing, nor a defiant choice. It is a mental health condition. No one sets out intentionally to become addicted to the chemicals or the behaviours.
By the time the person develops an addiction, their brain chemistry has already been significantly altered. The brain’s reward system, its memory pathways, its motivation circuits, its perception: all of these are changed in ways that make it extraordinarily difficult for the person to simply stop, even when they desperately want to. This is why you may hear your loved one promise they will quit and then not follow through.
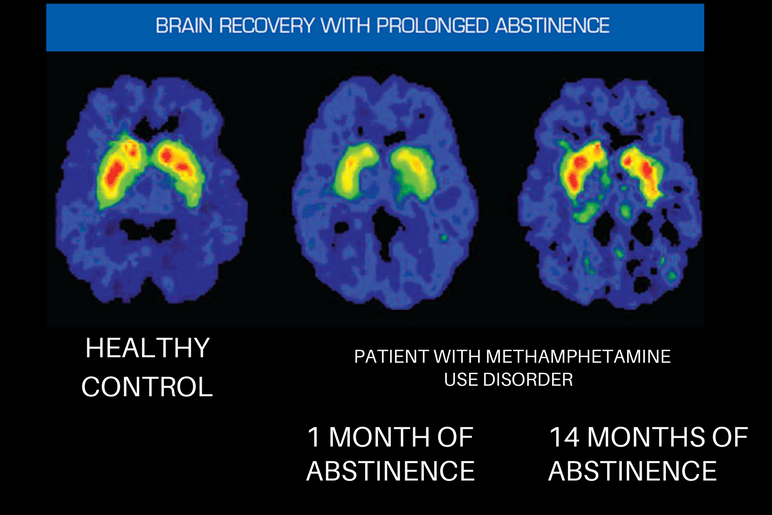
Source: National Institute on Drug Abuse https://nida.nih.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery
Their brains are running in a vicious loop, and they do not know how to get out of it. Further, they develop a sense of deep shame for not being able to free themselves from this mental prison, making it hard for them to receive any form of help, even when they know they need it. It is why they may lie, avoid, or act in ways that seem completely at odds with the person you know them to be.
Understanding the nature of addiction may help soften your emotions towards your loved ones and appreciate that the usual strategy of fervent reasoning or control is not going to be very effective. It does not mean we give up or be permissive, but we do have to adjust our strategies to create both emotional safety and momentum towards treatment.
Preparing Yourself for the Difficult Conversations
Before approaching your loved one for a difficult conversation, check in on your own emotional state. If you are in the grip of anger, resentment, or panic, or if your loved one is in the throes of their addiction, both parties will struggle to hear and connect with each other. Conversations tend to land better when the person initiating them is calm, clear, and coming from a place of genuine concern, and the person receiving them is momentarily free of the chemicals or the behaviours that are clouding their minds.
If more than one family member is speaking with the person affected, you would need to plan ahead on what each of you would be communicating and how this communication would be carried out. Do the work in researching treatment options and speak with relevant addiction professionals to help you craft your conversation. This would avoid overwhelming your loved one with either conflicting pieces of information or too much information. If there are family members who may not fully accept the condition of addiction or who may be emotionally triggered by the person, it may be best that they sit out the intervention conversation at this juncture. Focus on a unified approach before sitting down with your loved one for the conversation.
That said, you have to manage your expectations about the outcome of these conversations on treatment. The most well-prepared, well-timed, or the most heartfelt conversation may still not deliver the desired outcome with your loved one. It is important to recognise that one of the most powerful things you can do sometimes is to plant the seeds for change. Many people who eventually enter recovery point back to a conversation that did not seem to land at the time but stayed with them quietly, working beneath the surface and finding its way to their consciousness in rare moments of clarity.

You will likely have to deliver the intervention conversation more than once. To help you stay grounded throughout this process, you can practise emotional distancing or detachment from the expectations of outcome or any potential negative reactions to the conversations. This does not mean not caring for the person, but to create enough internal distance so that even if the conversation becomes heated, defensive, or painful, you can remain calm without taking the reactions personally. Remind yourself that you did not cause the addiction, you cannot cure it for your loved one, and you cannot control how the disease develops.
How to Approach the Conversation Itself
There is no universal script that works for every family, every relationship, every situation. But there are guiding principles that consistently make these conversations more effective.
Lead with love, and say it plainly. It may feel obvious to you that this conversation is happening because you care. But to your loved one, who is very likely carrying enormous shame and expecting judgment, it is not obvious at all. Say it directly: “I’m talking to you about this because I love you and I’m worried about you.” Say it more than once if you need to. Let it be the thread that runs through everything you do.
Use language that preserves dignity. Words matter enormously here. Avoid labels like “addict” and use “this addiction”; blame the disease, not the person. Avoid language that sounds judgemental, even if that is not your intention. Phrases like “you always,” “you never,” or “look what you have done” may feel accurate, but they activate shame, and shame is one of the most powerful drivers of continued substance use.
Avoid making the conversation about other members of the family: “Look at how you have hurt your mother” or “look at what you did to your siblings”. Instead, speak in terms of what you have observed about your loved one’s suffering and how it makes you feel. “I’ve noticed you seem to be struggling, and it worries me” lands very differently from “You have a problem and you need to fix it.”
Make room for your loved one to share their experiences. Listen more than you speak. On the surface, it may seem as if your loved one is so immersed in their addiction that nothing else seems to matter. Deep inside, they may be missing aspects of their lives that are no longer functional, hurting from lost relationships that they once treasured, grieving from the loss of their sense of self, or angry at themselves for not meeting their life’s potential.
“People struggling with addiction very often feel profoundly unheard.”
They live in a world of secrecy and isolation, and the experience of someone genuinely listening without interrupting, correcting, or steering towards a predetermined conclusion can be quietly transformative. This may be the most underrated piece of advice in the entire process.
You do not have to have all the answers at this moment. Sometimes what your loved one needs most is simply to feel that someone is willing to be present with the full, complicated truth of what they are going through. Offer unconditional presence. Let your loved one know that you will be there regardless of what happens next, whether they agree to seek help today, or whether the road ahead will have setbacks.
What to Avoid
Despite our best efforts, some of the most well-intentioned approaches can actually backfire. It is worth naming a few of them to minimise the emotional fallout.

Practising “tough love” in the form of scolding, threatening, or shaming the person almost never produces the result you are hoping for. Your loved one already feels terrible. Adding to that burden does not create motivation; it deepens the very emotional pain that drives the cycle of addiction. When a loved one is facing a health or medical crisis, it is important to still maintain a stance that balances compassion with clear, consistent boundaries. A supportive presence while upholding limits helps protect both the individual’s well-being and the relational dynamic.
Do not try to be their therapist. It is natural to want to fix things for someone you love. But addiction is a clinical condition that requires professional intervention. The most helpful thing you can do is encourage and support access to professional care. Focus your energy on what you can offer: emotional support, practical help, patience, and persistence.
If you are feeling overwhelmed and unable to hold a compassionate stance, please give yourself permission to take a step back. This does not mean that you are giving up on them; you are taking a much-needed pause so that you do not say words or do things that may hurt both of you further.
Understanding Your Treatment Options
One of the most empowering things you can do as a family member is arm yourself with knowledge about what treatment actually looks like. The landscape can feel overwhelming; there are outpatient programmes, inpatient residential programmes, therapy-based approaches, medication-assisted treatments, and various recovery support models. Terminology varies, websites are often vague, and it can be hard to know what to trust.
Our clinical team regularly navigates these complexities with families. We take a therapeutic, evidence-based approach and prioritise medical safety. You can learn more about The Winslow’s personalised residential program here.
Some Practical Steps That Can Help
Reach out to addiction treatment professionals directly. Do not rely solely on website descriptions. Call treatment centres and ask specific questions: What does a typical day of treatment look like? What therapeutic approaches do they use? What are the qualifications and experience of their clinical team? Is the facility licensed and regulated by a recognised health authority? A credible treatment provider will welcome these questions and answer them openly.
Ask about the level of care that would be appropriate for your loved one. Not everyone needs inpatient treatment, and not everyone can recover with outpatient support alone. An experienced addictions therapist can help you understand where your loved one falls on this spectrum based on the severity and duration of their addiction, their mental health, their social circumstances, and their readiness for change.
Look for experience and clinical depth. Addiction is complex and multifaceted. It frequently co-occurs with anxiety, depression, trauma, and other mental health conditions. Treatment that addresses only the surface behaviour without exploring what lies beneath it is less likely to produce lasting change. Look for programmes staffed by experienced professionals who can draw from multiple therapeutic approaches and tailor treatment to the individual.
Navigating the start of this process can feel overwhelming. Our multidisciplinary team of addiction specialists is here to provide clarity and help you determine the most appropriate next steps. If you would like to discuss your specific situation, you can schedule a confidential online consultation.
Don't Forget About Yourself
Here is something families often overlook in the urgency of helping their loved one: you need support too. Living with or caring about someone who has an addiction is emotionally draining. It reshapes your daily life, your sleep, your relationships, your sense of self. And over time, patterns develop — ways of coping, enabling, or absorbing stress — that can quietly erode your own wellbeing. It can also change the dynamics within the family system, creating secondary problems between family members, sometimes breaking families apart.
I strongly encourage family members to seek their own support, whether through individual therapy, family therapy, or support groups designed specifically for the loved ones of people in active addiction. These spaces offer something invaluable: the chance to learn, to share, and to discover things about your own patterns that you might not see on your own. Many family members who attend these groups describe moments of real revelation: realising, for instance, that behaviours they thought were helping were actually reinforcing the cycle, or that they had been neglecting their own needs for far longer than they realised.
Taking care of yourself is not selfish. It is, in fact, one of the most important things you can do for the person you are trying to help. A supported, grounded, emotionally resilient family member is a greater agent for change than one who is emotionally exhausted.
If You are Not Sure Where to Start
If all of this feels like a lot, let me simplify it.
You do not need to have the perfect conversation. You do not need to know everything about addiction or treatment before you start the conversation. You do need to show up with love, with kindness, and with the willingness to say: I see you. I am worried. I am here. And I would like to help you find support. That is enough to begin.

And if you need guidance on how to move forward, how to plan the conversation, what level of care to explore, or how to navigate the response you receive, reaching out to a professional who specialises in addiction and family support can make an enormous difference. You do not have to figure this out alone.
Recovery is possible. And it often begins not with the person who is struggling, but with the person who loves them enough to start the difficult conversation.
While this guide provides a foundation, every case is individual. To discuss your specific concerns, please contact our clinical team for a confidential discussion.